Abstract
Purpose
Postoperative ileus (POI) prolongs hospital stay and increases risk of postoperative complications. We conducted a randomized, sham-controlled trial to evaluate whether acupuncture reduces POI more effectively than sham acupuncture.
Methods
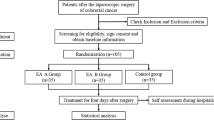
Colon cancer patients undergoing elective colectomy were randomized to receive 30 min of true or sham acupuncture twice daily during their first 3 postoperative days. GI-3 (the later of the following two events: time that the patient first tolerated solid food, AND time that the patient first passed flatus OR a bowel movement) and GI-2 (the later of the following two events: time patient first tolerated solid food AND time patient first passed a bowel movement) were determined. Pain, nausea, vomiting, and use of pain medications were evaluated daily for the first 3 postoperative days.
Results
Ninety patients were randomized. Eighty-one received the allocated intervention: 39 in the true acupuncture group and 42 in the sham acupuncture group, all evaluated for the primary endpoint. The mean time to GI-3 was 149 h [standard deviation (SD) 71 h] and 146 (SD 62 h) after surgery for the acupuncture group and the sham acupuncture group (difference between means −2 h; 95 % confidence interval −31, 26; p = 0.9). No significant differences were found between groups for secondary endpoints.
Conclusions
True acupuncture as provided in this study did not reduce POI more significantly than sham acupuncture. The study was limited by a standard deviation much larger than expected, suggesting that a study with a larger sample size might be required.

Similar content being viewed by others
References
Scott AM, Starling JR, Ruscher AE, et al. Thoracic versus lumbar epidural anesthesia’s effect on pain control and ileus resolution after restorative proctocolectomy. Surgery. 1996;120(4):688–95; discussion 695–7.
Liu SS, Carpenter RL, Mackey DC, et al. Effects of perioperative analgesic technique on rate of recovery after colon surgery. Anesthesiology. 1995;83(4):757–65.
Holte K, Kehlet H. Postoperative ileus: progress towards effective management. Drugs. 2002;62(18):2603–15.
Delaney CP, Weese JL, Hyman NH, et al. Phase III trial of alvimopan, a novel, peripherally acting, mu opioid antagonist, for postoperative ileus after major abdominal surgery. Dis Colon Rectum. 2005;48(6):1114–25; discussion 1125–6; author reply 1127–9.
Wolff BG, Michelassi F, Gerkin TM, et al. Alvimopan, a novel, peripherally acting mu opioid antagonist: results of a multicenter, randomized, double-blind, placebo-controlled, phase III trial of major abdominal surgery and postoperative ileus. Ann Surg. 2004;240(4):728–34; discussion 734–5.
Purkayastha S, Tilney HS, Darzi AW, et al. Meta-analysis of randomized studies evaluating chewing gum to enhance postoperative recovery following colectomy. Arch Surg. 2008;143(8):788–93.
Wolff BG, Viscusi ER, Delaney CP, et al. Patterns of gastrointestinal recovery after bowel resection and total abdominal hysterectomy: pooled results from the placebo arms of alvimopan phase III North American clinical trials. J Am Coll Surg. 2007;205(1):43–51.
Kaptchuk TJ. Acupuncture: theory, efficacy, and practice. Ann Intern Med. 2002;136(5):374–83.
Balestrini JL, Tsuchida D, Fukuda H, et al. Acupuncture accelerates delayed gastrointestinal transit after abdominal surgery in conscious rats. Scand J Gastroenterol. 2005;40(6):734–5.
Sugai GC, Freire Ade O, Tabosa A, et al. Serotonin involvement in the electroacupuncture- and moxibustion-induced gastric emptying in rats. Physiol Behav. 2004;82(5):855–61.
Tabosa A, Yamamura Y, Forno ER, et al. Effect of the acupoints ST-36 (Zusanli) and SP-6 (Sanyinjiao) on intestinal myoelectric activity of Wistar rats. Braz J Med Biol Res. 2002;35(6):731–9.
Choi M, Jung J, Seo M, et al. Ultrasonographic observation of intestinal mobility of dogs after acupunctural stimulation on acupoints ST-36 and BL-27. J Vet Sci. 2001;2(3):221–6.
Chou JW, Chang YH, Chang CS, et al. The effect of different frequency electrical acu-stimulation on gastric myoelectrical activity in healthy subjects. Hepatogastroenterology. 2003;50(50):582–6.
Chang CS, Ko CW, Wu CY, et al. Effect of electrical stimulation on acupuncture points in diabetic patients with gastric dysrhythmia: a pilot study. Digestion. 2001;64(3):184–90.
Chen LL, Hsu SF, Wang MH, et al. Use of acupressure to improve gastrointestinal motility in women after trans-abdominal hysterectomy. Am J Chin Med. 2003;31(5):781–90.
Liu JX, Zhao Q. Effect of acupuncture on intestinal motion and sero-enzyme activity in perioperation. Zhong Xi Yi Jie He Za Zhi. 1991;11(3):156–7, 133–4.
Wan Q. Auricular-plaster therapy plus acupuncture at Zusanli for postoperative recovery of intestinal function. J Tradit Chin Med. 2000;20(2):134–5.
Meng ZQ, Garcia MK, Chiang JS, et al. Electro-acupuncture to prevent prolonged postoperative ileus: a randomized clinical trial. World J Gastroenterol. 2010;16(1):104–11.
Lao L, Bergman S, Langenberg P, et al. Efficacy of Chinese acupuncture on postoperative oral surgery pain. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995;79(4):423–8.
Kaptchuk TJ, Stason WB, Davis RB, et al. Sham device v inert pill: randomised controlled trial of two placebo treatments. BMJ. 2006;332(7538):391–7.
Acknowledgment
The authors thank Maria Kryza, Stacey Guillen, Derek Woo, James Lozada, Gria Jacobs, and Kristofer Prepelica for their assistance in the conduct of the study and the preparation of the manuscript. The study was supported by the National Institutes of Health grant number R21CA122199.
Conflict of interest
No commercial interest is disclosed.
Author information
Authors and Affiliations
Corresponding author
Additional information
W. Douglas Wong—Deceased January 20, 2011
Rights and permissions
About this article
Cite this article
Deng, G., Wong, W.D., Guillem, J. et al. A Phase II, Randomized, Controlled Trial of Acupuncture for Reduction of Postcolectomy Ileus. Ann Surg Oncol 20, 1164–1169 (2013). https://doi.org/10.1245/s10434-012-2759-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2759-7