Abstract
Purpose
This double-blind randomized controlled trial was conducted to evaluate whether use of acupuncture could initiate labor at term and thus reduce post-term induction.
Methods
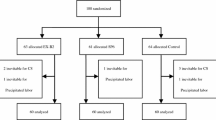
Between 2010 and 2011, a total of 80 women at 38 weeks of gestation or greater were randomized to acupuncture and sham acupuncture groups. Acupuncture points LI4, SP6 and BL67 were needled bilaterally. The primary outcome was initiation of labor. The time from acupuncture to delivery, mode of delivery, fetal and maternal outcome and Apgar scores were recorded. The trial is registered at irct.ir, number IRCT201111218151N1.
Results
Eighty women were randomized and 75 women completed the study procedure. Age, BMI, parity and gestational age were similar in both groups. Spontaneous labor was initiated in 94.7 % of acupuncture group and 89.2 % of sham acupuncture group (p = 0.430). There were no statistically significant difference between groups for time from enrollment to delivery (p = 0.06).
Conclusion
According to this study, it seems that acupuncture was not effective in labor initiation compared to sham acupuncture.

Similar content being viewed by others
Abbreviations
- RCT:
-
Randomized controlled trail
- BMI:
-
Body mass index
- LI4:
-
Large intestine 4
- SP6:
-
Spleen 6
- BL67:
-
Bladder 67
- GA:
-
Gestational age
- NVD:
-
Normal vaginal delivery
- ACOG:
-
American College of Obstetricians and Gynecologists
References
Dencker A, Berg M, Berggvist L, Ladfors L, Thorsen LS, Lilja H (2009) Early versus delayed oxytocin augmentation in nulliparous women with prolonged labour—a randomized controlled trial. BJOG 116(4):530–536
Mozurkewich EL, Chilimigars JL, Berman DR, Perni UC, Romero VC, King VJ, Keeton KL (2011) Methods of induction of labour: a systematic review. BMC Pregnancy Childbirth 11:84
Asher GN, Coeytoux RR, Chen W, Reilly AC, Loh YL, Harper TC (2009) Acupuncture to initiate labor: a randomized, sham controlled clinical trial. J Matem Fetal Neonatal Med 22(10):843–848
Caughey AB, Sundaram V, Kaimal AJ, Gienger A, Cheng YW, McDoland KM, Shaffer BL, Owens DK, Bravata DM (2009) Systematic review: elective induction of labor versus expectant management of pregnancy. Ann Intern Med 151:252–263
Alexander JM, McIntire DD, Leveno KJ (2001) Prolonged pregnancy: induction of labor and cesarean birth. Obstet Gynecol 97(6):911–915
Arrowsmith S, Quenby S, Weeks A, Burdyga T, Wray S (2012) Poor spontaneous and oxytocin-stimulated contractility in human myometrium from postdates pregnancies. PLoS One 7(5):e36787
Wennerholm UB, Hagberg H, Brorsson B, Bergh C (2009) Induction of labor versus expectant management for post-date pregnancy: is there sufficient evidence for a change in clinical practice? Acta Obstet Gynecol Scand 88(1):6–17
Smith CA, Crowther CA (2004) Acupuncture for induction of labour. Cochrance Database Sys Rev (1):CD002962
Selmer-Olsen T, Lydersen S, Morkved S (2007) Does acupuncture used in nulliparous women reduce time from prelabour rupture of membranes at term to active phase of labour? A randomised controlled trial. Acta Obstet Gynecol Scand 86:1447–1452
Gaudet LM, Dyzak R, Aung SK, Smith GN (2008) Effectiveness of acupuncture for the initiation of labour at term: a pilot randomized controlled trial. J Obstet Gynaecol Can 30(12):1118–1123
MacPherson H, Thomas K, Walters S, Fitter M (2001) The York Acupuncture Safety Study: prospective survey of 34 000 treatments by traditional acupuncturists. BMJ 323:486–487
Lao L, Hamilton GR, Fu J, Berman BM (2003) Is acupuncture safe? A systematic review of case reports. Altern Ther Health Med 9:72–83
Smith CA, Cochrance S (2009) Dose acupuncture have a place as an adjunct treatment during pregnancy? A review of randomized controlled trials and systematic reviews. Birth 36(3):246–253
Tiran D (2004) Breech presentation: increasing maternal choice. Complement Ther Nurs Midwifery 10(4):233–238
Qu F, Zhou J (2007) Electro-acupuncture in relieving labor pain. Evid Based Complement Alternat Med 4(1):125–130
Helmreich RJ, Shiao SY, Dune LS (2006) Meta-analysis of acustimulation effects on nausea and vomiting in pregnant women. Explore (NY) 2(5):412–421
Gaudernack LC, Forbod S, Hole E (2006) Acupuncture administered after spontaneous rupture of membranes at term significantly reduces the length of birth & use of oxytocin. A randomized controlled trial. Acta Obstetrica et Gynecologia Scandinavica 85(11):1348–1353
Smith CA, Crowther CA, Collins CT, Coyle ME (2008) Acupuncture to induce labor: a randomized controlled trial. Obstet Gynecol 112(5):1067–1074
Citkovitz C, Klimenko E, Bolyai M, Applewhite L, Julliard K, Weiner Z (2009) Effects of acupuncture during labor and delivery in a U.S hospital setting: a case-control pilot study. J Altern Complement Med 15(5):501–505
Evans M (2009) Postdates pregnancy and complementary therapies. Complement Ther Clin Pract 15(4):220–224
Harper TC, Coeytoux RR, Chen W, Campbell K, Kaufman JS, Moise KJ, Thorp JM (2006) A randomized controlled trail of acupuncture for initiation of labor in nulliparous women. J Matern Fetal Neonatal Med 19(8):465–470
Tempfeer C, Zeisler H, Heinzl H, Hefler L, Husslein P, Kainz C (1998) Influence of acupuncture on maternal serum levels of interleukin-8, prostaglandin F2 alpha, and beta-endorphin: a matched pair study. Obstet Gynecol 92(2):245–248
Norwitz ER, Snegovskikh VV, Caughey AB (2007) Prolonged pregnancy: when should we intervene? Clin Obstet Gynecol 50(2):547–557
Olesen AW, Basso O, Olsen J (2003) Risk of recurrence of prolonged pregnancy. BMJ 326(7387):476
Kistka ZA, Palomar L, Boslaugh SE, DeBaum MR, DeFranco EA, Muglia LJ (2007) Risk for postterm delivery after previous postterm delivery. Am J Obstet Gynecol 196(3):241.e1–241.e6
Rabl M, Ahner R, Bitschanau M, Zeisler H, Husslein P (2001) Acupuncture for cervical ripening & induction of labor at term—a randomized controlled trial. Wein Klin Wochenschr 113(23–24):942–946
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ajori, L., Nazari, L. & Eliaspour, D. Effects of acupuncture for initiation of labor: a double-blind randomized sham-controlled trial. Arch Gynecol Obstet 287, 887–891 (2013). https://doi.org/10.1007/s00404-012-2674-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-012-2674-y